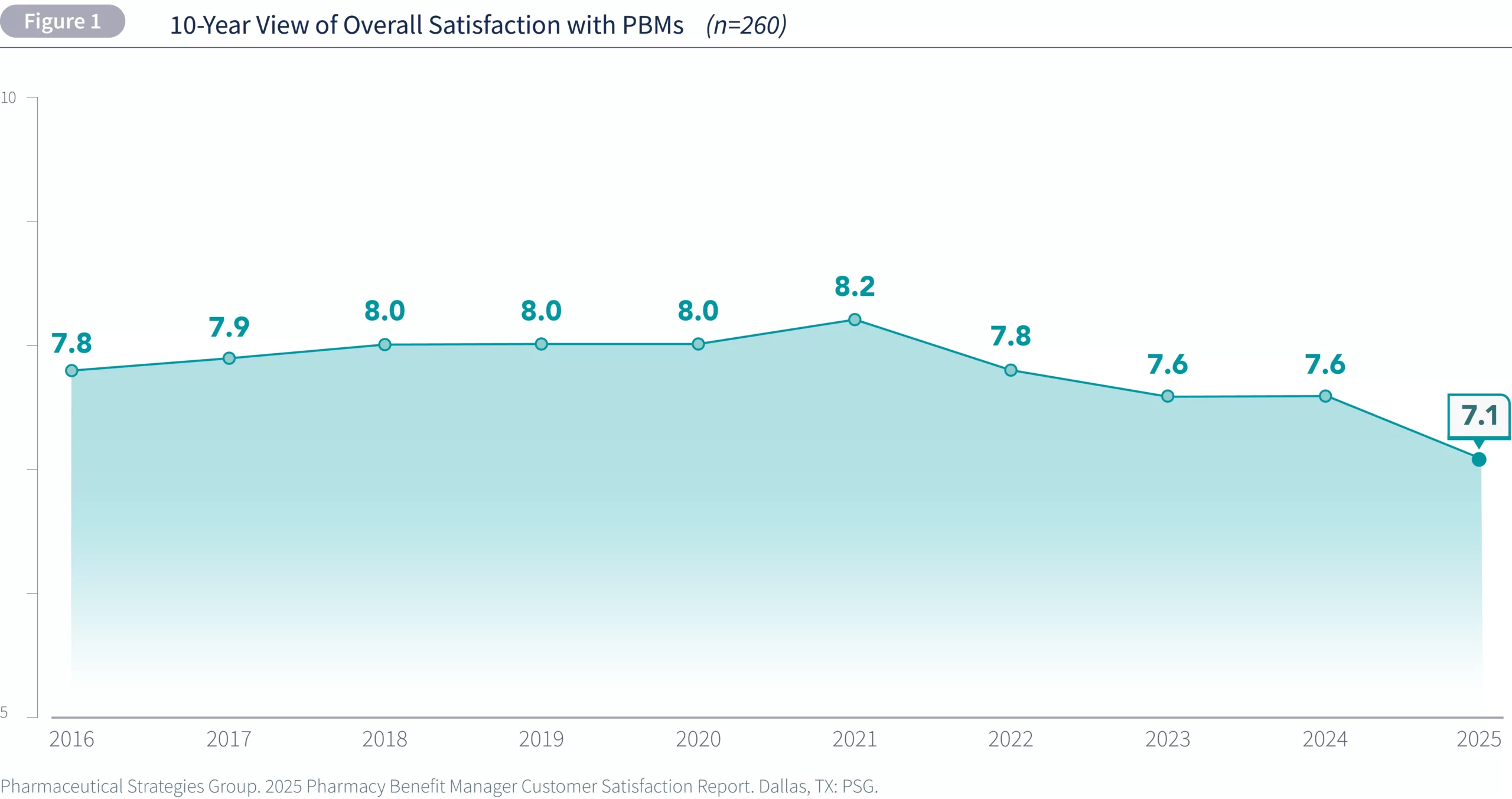
Choosing a pharmacy benefit manager is not just a cost decision. It shapes access, member experience, formulary design, specialty drug handling, and the day-to-day burden on HR teams. In practice, the Best PBMs are the ones that combine clear pricing, strong service, broad network support, and measurable plan performance instead of relying on headline promises alone. PBMs manage prescription drug benefits for insurers and employers by handling formularies, claims, networks, rebates, and mail-order services, which is why their impact reaches far beyond the pharmacy counter.
That is also why there is no single universal scoreboard that settles the question forever. A PBM can look strong on one measure and average on another. One may be excellent at scale, another at service, and another at transparency. For that reason, the most useful way to compare Best PBMs is to look at overall plan performance as a blend of cost control, member access, satisfaction, accountability, and contract clarity. Recent industry reports show how concentrated the market remains and how satisfaction is measured through multiple dimensions rather than one simple number.
What a PBM Actually Does
A PBM sits between the health plan, the employer, the pharmacy, and the drug manufacturer. Its job is to administer prescription benefits and help decide which drugs are covered, how much members pay, and how claims are processed. PBMs also negotiate with pharmacies and manufacturers, manage pharmacy networks, and support mail-order and specialty pharmacy services. That makes the PBM one of the most influential players in prescription drug access and spending.
The core responsibilities that matter most
When an employer or plan sponsor evaluates a PBM, the important questions are practical. Does the PBM make prescriptions easier to access? Does it hold down net cost, not just list cost? Does it explain pricing clearly? Does it support members when a drug is switched, rejected, or delayed? These questions matter because PBM design can affect both savings and member satisfaction. Industry guidance on PBM contracting and evaluation consistently emphasizes financial analysis, contractual terms, and the way the PBM actually performs after implementation.
How to Read Overall Plan Performance Ratings
The phrase overall plan performance ratings sounds simple, but in pharmacy benefits it usually combines several signals. A strong rating should reflect more than rebate volume or the number of covered drugs. It should include transparency, pricing accuracy, access to medication, network breadth, response speed, and the ability to support a plan’s clinical goals. The most reliable rating approach is one that checks both hard financial results and lived member experience. That is why satisfaction surveys and plan-performance frameworks are often more useful together than separately.
Transparency
Transparency is one of the biggest dividing lines among PBMs. A PBM may advertise savings, but the real question is whether the employer can see how the savings are created, what is retained, and what is passed through. Evaluation guides and performance metric explainers repeatedly warn that hidden pricing methods can make a plan look better on paper than it truly is. Transparency matters because it helps buyers compare net cost instead of being distracted by surface-level discounts.
Cost control
The next layer is cost control. Good PBMs do not simply push the cheapest product in every case; they create a balance between affordability, clinical appropriateness, and continuity of care. Cost control becomes especially important when specialty drugs and long-term therapies are involved. Current market reports show the PBM space remains enormous and highly concentrated, which means even small performance differences can affect very large populations and very large budgets.
Access and service
Access is often where plan performance becomes personal. Members do not experience a PBM as an abstract pricing engine. They experience it as whether a medicine is covered, whether a prior approval is processed quickly, whether a pharmacy is in network, and whether a refill arrives when expected. Customer satisfaction reports for PBMs track these experiences because they shape retention, recommendation, and renewals. In 2025, PSG reported that high-level PBM satisfaction declined and that the supplement includes ratings for transparency, likelihood to recommend, and reasons for selection across several major PBMs.
Clinical quality and safety
A high-performing PBM should also support clinical quality. That means helping plans manage formularies, avoid unnecessary utilization, and direct members toward safe, effective therapy choices. The best rating systems do not treat this as a side issue. They check whether clinical management supports outcomes without adding avoidable friction. This is one reason buyers should look at the PBM’s utilization management process, specialty support, and how it handles appeals and exceptions.
Which PBMs Tend to Rank Near the Top
When people ask about the Best PBMs, they usually mean the firms with the strongest overall combination of market position, service footprint, and plan performance. Recent industry coverage shows that the market is still dominated by three major companies: CVS Caremark, Express Scripts, and Optum Rx. Drug Channels estimated that in 2025 these three processed about 80% of equivalent prescription claims, which shows how concentrated the space remains. That concentration does not automatically make any one PBM perfect, but it does show where most employers are still looking first.
The big three and what they represent
The largest PBMs usually appeal to buyers that value scale, network depth, and broad administrative capability. Their size gives them leverage in contracting and makes them relevant for large employer groups, national plans, and organizations that want a single platform for complex pharmacy operations. At the same time, large size can come with scrutiny, especially when buyers want more visibility into pricing and stronger alignment between claims, rebates, and member outcomes.
Strong alternatives beyond the largest names
The strongest alternatives often include Prime Therapeutics, Navitus, and MedImpact, especially for employers who want a more customized service model or a different transparency structure. PSG’s 2025 satisfaction supplement specifically includes CVS Health, Express Scripts, OptumRx, MedImpact, Navitus, and Prime Therapeutics among the PBMs with sufficient responses for detailed ratings. That is useful because it shows buyers where meaningful comparisons can be made beyond the largest three.
Why the “best” label depends on the plan
A PBM that is excellent for a very large self-funded employer may not be the best fit for a smaller organization. Likewise, a PBM that performs well on access may not be the best for a plan trying to maximize transparency. This is why the phrase Best PBMs should always be read as “best for a specific plan design, member base, and budget strategy,” not as one permanent universal ranking.
A Practical Way to Compare PBMs Fairly
If you are trying to compare vendors, the smartest approach is to use a scorecard that blends business, clinical, and member factors. That scorecard should favor measurable outcomes over marketing language. It should also separate gross savings from net savings, because the two are not the same. PBM evaluation resources consistently recommend looking closely at contract terms, performance guarantees, and the way the PBM reports results over time.
1) Start with net cost, not headline discounts
A strong PBM should be able to show what the employer actually pays after pricing rules, rebates, and administrative details are applied. Headline discounts are not enough. The plan sponsor should understand whether the savings are passed through cleanly or blurred by spread pricing, clawbacks, or unclear reconciliation methods. This is one of the most important distinctions in modern PBM evaluation.
2) Review formulary design carefully
Formularies should support good care and fair access. They should not be so restrictive that members face unnecessary barriers, but they should still encourage appropriate use of effective lower-cost options. PBMs shape formularies directly, so plan sponsors need to know how exclusions, tiering, and utilization controls are decided. The right balance can improve both plan performance and member experience.
3) Check service quality under pressure
A PBM looks very different when everything is going smoothly versus when a member is trying to fill a time-sensitive prescription. Service quality should be tested during exceptions, coverage changes, refill problems, and specialty drug transitions. A vendor that is calm and responsive in these moments usually deserves a higher overall rating than one that only looks efficient on a spreadsheet.
4) Ask how specialty drugs are handled
Specialty medications are one of the biggest drivers of pharmacy cost and complexity. The PBM should explain how it supports prior approvals, specialty fulfillment, adherence, and clinical monitoring. A plan that ignores specialty management may not see the full impact of its PBM, even if the standard claims report looks good.
5) Compare reporting depth
A PBM should provide more than a monthly invoice and a few summary charts. Buyers should expect reporting that makes trends easy to understand, including utilization, cost shifts, member disruption, and therapeutic changes. The best vendors can explain not only what changed, but why it changed. That level of clarity is one of the main signs of a strong overall plan performer.
When a Big PBM Makes Sense
For some organizations, the scale of the big national PBMs is a real advantage. A very large employer may need broad pharmacy access, deep integration with other benefits, and highly standardized claims processing. In those situations, large PBMs can offer strong operational consistency and wide network support. That is especially important when the employer values national consistency more than boutique customization.
Best fit for nationally distributed workforces
If employees are spread across many states, a larger PBM may simplify plan administration. A broader network can reduce friction for members who travel, relocate, or use multiple pharmacy channels. Large PBMs are often better positioned to serve that kind of dispersed population because of their scale and contracting reach.
Best fit for more complex benefit designs
Some employers use multiple plan designs, specialty carve-ins, or layered pharmacy rules. In those cases, a PBM with mature systems and large operational capacity may be easier to configure. That does not automatically make it the winner, but it does make it more competitive for organizations with complicated needs.
When a Smaller or More Transparent PBM Can Win
A smaller or more transparent PBM can shine when the employer wants clear reporting, stronger service relationships, and simpler contract language. These vendors may not dominate the market share charts, but they can still deliver excellent outcomes for the right client. The key is alignment. A transparent PBM that matches a plan’s goals may outperform a larger competitor that looks impressive in the abstract but adds friction in practice.
Best fit for buyers who value clarity
Employers that want a direct view into pricing and utilization often prefer models that emphasize straightforward fee structures and cleaner contract terms. This makes it easier for finance and benefits teams to understand where every dollar is going and to explain that story internally.
Best fit for service-sensitive groups
Some groups care more about service quality than about pure scale. A PBM that responds quickly, communicates clearly, and resolves issues with fewer handoffs can be a stronger overall performer for those clients. That is one reason customer satisfaction data belongs in any real ranking of the Best PBMs.
Red Flags That Lower a PBM’s Overall Rating
A weak PBM often leaves clues before the contract is signed. Vague pricing, hard-to-read guarantees, and evasive answers about rebates are all warning signs. So are reports that do not make it easy to separate the plan’s true cost from the PBM’s retained value. Industry evaluation guides consistently stress that buyers should scrutinize contract terms and performance measurement closely before committing.
Warning sign: too much emphasis on one metric
A PBM that only talks about rebates, or only talks about service, is not giving the whole picture. Overall plan performance requires balance. When one metric is used to distract from another, buyers should slow down and ask for a fuller picture.
Warning sign: unclear member impact
A contract can look attractive on paper while quietly creating refill delays, coverage confusion, or unnecessary step edits for members. If the PBM cannot explain how the plan experience will actually feel, that is a problem. The best evaluations treat member impact as a first-class metric, not an afterthought.
Warning sign: limited reporting after launch
Some PBMs are strong during the sales process but weak once the plan is live. If reporting is shallow, late, or hard to interpret, it becomes difficult to know whether the PBM is truly delivering value. Reliable ongoing reporting is one of the strongest signs of a high-performing partner.
A Simple Employer Scorecard You Can Use
A practical scorecard helps turn a complex buying process into something manageable. The best way to do this is to rate each vendor on a few major dimensions and then compare the total picture. A simple model can include transparency, net cost, access, service, clinical controls, and reporting. That kind of balanced approach mirrors how broader health-plan rating systems evaluate performance and satisfaction together.
You can think of the scorecard in three layers. First comes cost efficiency, which includes net price and rebate handling. Second comes member experience, which includes access, service, and communication. Third comes governance, which includes reporting, accountability, and the ability to explain decisions clearly. A PBM that does well in all three layers is usually the strongest overall choice.
This is also where the phrase Best PBMs becomes practical rather than promotional. The winner is not the vendor with the loudest claim. It is the one that performs best against the plan’s real goals, under real-world conditions, with documentation that can stand up to review.
For a plain-language overview of the topic, see Pharmacy benefit management on Wikipedia.
Final Thoughts
A strong PBM is not defined by size alone, and it is not defined by a single discount number. The real measure is whether it delivers clear pricing, accessible benefits, dependable service, and measurable value across the full plan year. The market remains highly concentrated, with the largest share still held by CVS Caremark, Express Scripts, and Optum Rx, but satisfaction and performance still vary enough that buyers should compare carefully instead of assuming one name is automatically the answer.